As Colorectal Disease Awareness Month approaches this March, it’s important to know that regular colonoscopy can prevent colorectal cancer by detecting and removing precancerous polyps. With regular screening, you can proactively manage these developments and reduce your risk of colorectal cancer.
V. Carlos Arcos, MD, is a board-certified colorectal surgeon at INTEGRIS Health Baptist Medical Center. Here are answers to some frequently asked questions about colonoscopy.
How does a colonoscopy work: A colonoscope uses a long flexible tube with a small camera on the end. It helps detect and prevent problems by removing growths before they become cancerous.
You can sleep comfortably on your left side. An anesthesiologist will administer mild anesthesia through an IV. With this method, you can sleep safely without any pain or discomfort.
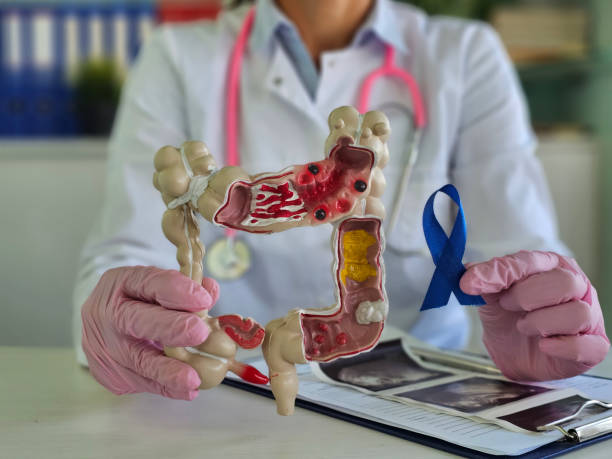
Next, the doctor inserts the colonoscope into the rectum and guides it through the rectum and large intestine (colon).
This camera helps detect any abnormalities in the colon such as polyps, masses or tumors.
Any polyps or suspicious areas are removed using a small instrument or biopsy.
If your doctor finds cancerous tissue, a biopsy will help the pathologist collect a tissue sample.
The entire process usually takes 30 minutes, but some take anywhere from 15 or 45 minutes to an hour.
Colonoscopy preparation: Colonoscopy preparation is critical to the success of the procedure and often includes dietary changes and colon hygiene procedures to provide a clear view of the colon.
Following a low-fiber diet in the days before the test will slow down bowel movements. Low-fiber foods include white bread, white pasta, white rice, lean protein, or whole vegetables.

Start a clear liquid diet the day before your colonoscopy. Examples include water, clear sauce, gelatin, or popsicles (no colors or additives).
The stool will be removed the night before oral surgery. There are many types of pre-colonoscopy solutions, but the most common are osmotic laxatives and electrolytesOsmotic laxatives draw more water into the colon to soften the stool and stimulate the muscles.
Fluid loss from frequent bowel movements can lead to dehydration. Electrolytes help replenish important nutrients such as sodium, calcium and potassium.
Polyethylene glycol (PEG) 3350 (sold under the brand names Golitely, Nulitely, Movieprep, etc.) is the most common type of latex.
Enteral PG preparations are gentle on intestinal tissue but require large volumes of fluid (up to 4 L) for ingestion.
A sodium phosphate laxative (such as SUPREP) requires a small amount of liquid (96 oz).
Discuss with your doctor which combination is right for you.
Many people fear colonoscopy. To put your mind at ease, read this simple guide to colorectal cancer screening.
Importance of colorectal cancer screening.
Bottom Line: Next to skin cancer, colorectal cancer is the leading cause of death in the United States. Colonoscopy can help reduce deaths related to colorectal cancer, the third most common cancer in men and women.
Over time, colon polyps, or abnormal polyps, can turn into colon cancer. Early detection and screening can improve treatment success by detecting and removing benign tumors before they turn cancerous.
If colon cancer is detected early, the cure rate for colon cancer can exceed 90%.Colon cancer is a slow-growing cancer, and most polyps can take 10 to 15 years to become cancerous.
Colonoscopy is more accurate than home screening tests for detecting colorectal cancer (95% vs. 92% with ColonGuard).
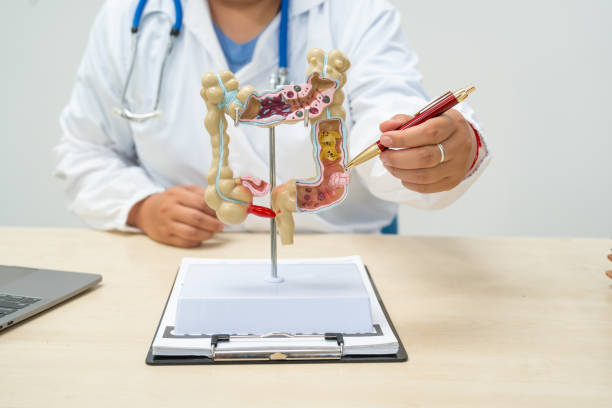
Type of test
There are several screening tests to detect polyps or colorectal cancer. The task force identified the following colorectal cancer screening strategies: For certain screening tests (stool examination, flexible sigmoidoscopy, CT colonography), it is important to know that if the test results are positive or abnormal, a microscopic examination of the colon is required. Complete the screening process. Talk to your doctor about which test is right for you.
Stool examination: The GAK-based occult blood test (GFOBT) uses the chemical GAK to detect blood in the stool. Do this once a year. For this test, you will receive a test kit from your healthcare provider. At home, they use a stick or brush to remove small droppings. The test kit is sent back to the doctor or laboratory to test the stool sample for blood.
Faecal immunoassay (FIT) uses antibodies to detect blood in the stool. The GFOBT is held annually.
FIT-DNA testing (also called stool DNA testing) combines FIT with a test that looks for DNA changes in stool. To run the test, they collected all the stool and sent it to a lab, where it was analyzed for DNA and blood changes conducted every 3 years.
Flexible sigmoidoscopy: To perform this test, your doctor will insert a small, flexible, lighted tube into your rectum. The doctor will examine the rectum and lower third of the colon for polyps or cancer.
Frequency: Every 5 or 10 years as appropriate.
Reference
https://www.cdc.gov/colorectal-cancer/screening/index.html#:~:text=Colorectal%20cancer%20almost%20always%20develops,early%2C%20when%20treatment%20works%20best.
https://ufhealth.org/stories/2024/the-importance-of-colorectal-cancer-screening-how-early-detection-saves-lives
http://www.bccancer.bc.ca/screening/colon/who-should-screen/why-colon-screening-is-important
https://www.cancercare.org/publications/116-colorectal_cancer_understanding_risk_factors_and_screening
https://www.mayoclinic.org/diseases-conditions/colon-cancer/in-depth/colon-cancer-screening/art-20046825
https://bestcare.org/news/importance-colorectal-cancer-screening
https://medlineplus.gov/ency/article/002071.htm
https://integrishealth.org/resources/on-your-health/2024/march/colon-cancer-screening
https://fascrs.org/patients/diseases-and-conditions/a-z/screening-and-surveillance-for-colorectal-cancer-e
https://amp.cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/screening-tests-used.html#amp_tf=From%20%251%24s&aoh=17267374118371&referrer=https%3A%2F%2Fwww.google.com
 using WordPress and
using WordPress and
Comments are closed